|
 |
- Search
| Asian J Kinesiol > Volume 23(4); 2021 > Article |
|
Abstract
OBJECTIVES
The purpose of this study was to analyze the effects of brief dry cupping on muscle soreness of the gastrocnemius muscle and range of motion (ROM) in the ankle.
METHODS
Thirty-six participants (age=29┬▒10 yrs, ht=173.8┬▒10.3 cm, wt=75.3┬▒15.9 kg) were randomly assigned to three groups: A (no exercise), B (bilateral heel drops to exhaustion), and C (right unilateral heel drops to exhaustion). Dorsiflexion ROM was assessed bilaterally for all groups. All participants received the cupping protocol on the right gastrocnemius, but C also received it on the left. Dry cupping was applied using four two-inch cups in four quadrants on the calf for 90 seconds. Soreness was reported using a 10-point VAS scale at 24- and 48-hours. Repeated measures ANOVAs were used to examine the effects of cupping on soreness and range of motion, respectively. Alpha was set at 0.05 for all tests.
RESULTS
A significant difference in muscle soreness existed between right (3.58┬▒1.31 VAS) and left (2.83┬▒1.02 VAS) calves for group B at 24 hours (p = 0.029). No other significant differences existed between calves that were and were not cupped (p > 0.05). No significant differences in ROM occurred between any conditions (p > 0.05).
The common term used to describe muscle soreness after exercise is delayed onset muscle soreness (DOMS), which is characterized by mild to severe tenderness or stiffness with movement or palpation [1]. This soreness typically increases within the first 24 hours after exercise, peaking between 24 and 72 hours, and subsiding thereafter [2]. While the mechanisms of DOMS are not entirely clear, some have postulated the soreness could be due to lactic acid accumulation, muscle spasms, connective tissue damage, muscle damage, inflammation, and/or enzyme efflux [3]. Eccentric exercises and unaccustomed exercises that are different from the normal activity for that individual are the most common cause of DOMS [3-9].
In addition to tenderness and stiffness, the resulting pain, inflammation, reduction in force generation, and limited range of motion (ROM) associated with DOMS [3-5,10,11] can lead to injury caused by muscle damage and change in gait patterns if it persists [7,9]. For example, DOMS reduces ROM in the knee and ankle joints by 3.2% [7], thereby affecting locomotion and possibly reducing participation in physical activity. Experiencing DOMS can lower the quality of life and can causes avoidance of activities that maintain a healthy lifestyle.
While DOMS is the most widely studied type of muscle soreness, other types of muscle soreness have also been identified. For example, acute exercise-induced muscle soreness is perceived pain during and immediately after exercise, and has been thought to be caused by muscle ischemia [12]. Others have used the term immediate-onset muscle soreness (IOMS), which is associated with stiffness, aching pain, and tenderness [13], and has been characterized as that which occurs after completing long-term exercise [14]. Symptoms of IOMS typically last for only hours and are relatively transient compared to those of DOMS [13]. Whether the muscle soreness due to exercise is acute or delayed, the degree of pain and limitations, as well as the means to relieve symptoms, are similar between the two with the main difference being when the symptoms are presented [13]. This may be due in part to acid sensing ion channels, which are found in muscle afferents, and thought to play a role in different pain conditions. It has been reported these ion channels may play a role in the pain associated with IOMS [15], whereas in DOMS they are not [16].
Regardless of the time-course of pain, muscle soreness can deter one from exercising or can hamper training programs, and many methods have explored techniques to reduce this soreness. Prevention and treatment strategies for muscle soreness vary and new ways to avoid and combat it are continually investigated. For example, approaches to remedying the effects of muscle soreness include massage [11,17-18], stretching [18,19], foam rolling [20,21], acupuncture [22-24], ointments [6,25], non-steroidal antiinflammatory drugs [3,25], and exercise [11,26], but no technique has been found to alleviate the discomfort in its entirety. Finding a treatment method that provides quick and lasting relief from the symptoms of muscle soreness would be beneficial for any who would experience it.
One such method, cupping therapy, started in eastern medicine many centuries ago in part to treat various diseases [27]. It is an ancient technique closely related to acupuncture, dry needling, and myofascial release techniques. The technique for dry cupping places cups on the skin superficial to the skeletal muscle affected with negative pressure, creating a vacuum that lifts the soft tissue and fascia in the region to create a stretch in the surrounding tissues and muscles. Wet cupping similarly employs the same technique but includes small incisions in the skin underneath the cups. The practice has been used for decades by many without much supporting scientific research. Claims of cupping therapy include improved pain relief and ROM, faster healing, reduced inflammation, enhanced sports performance, and faster recovery exist, but without much scientific review. Some research supports the claims [28-35], but others suggest cupping effects are inconclusive [36,37]. If dry cupping can reduce inflammation, relieve pain, increase ROM, and minimize recovery time, the technique may result in a decrease in muscle soreness and thereby be valuable in recovery and rehabilitation situations. The purpose of this study was to investigate the effects of a single brief bout of dry cupping therapy on muscle soreness and ROM on the gastrocnemius muscle and ankle joint after strenuous exercise. It was hypothesized that dry cupping would decrease the effects of muscle soreness in the calf and increase ROM for dorsiflexion.
This study was reviewed and approved by the UniversityŌĆÖs Institutional Review Board (#2019-43). To calculate the sample size, the ANOVA with repeated measures and within-between interaction was employed with three groups, four measurements, an alpha rate of 0.05, power of 0.80 (80%), and an effect size of 0.25 (G*Power v 3.1.9) [38]. Based on this, a sample size of 10 was indicated for each group for a total of 30, whereas 12 was used for each group to account for attrition.
Participants signed a written informed consent before the study began. Participant exclusion included lower-limb injuries or skin conditions, unaccustomed lower extremity exercise 24 hours to participation, allergies to olive oil or plastic, pregnancy, blood disorders, or use of blood thinning medication. Participants were instructed to not use anti-inflammatory and pain relief medications, or consume supplements (such as pre-workout drinks) 24-hrs prior and for the duration of the study. Participants were also instructed to remove any hair from the calf to be cupped prior to reporting to the lab. Hair trimmers were available if needed on the day of the study.
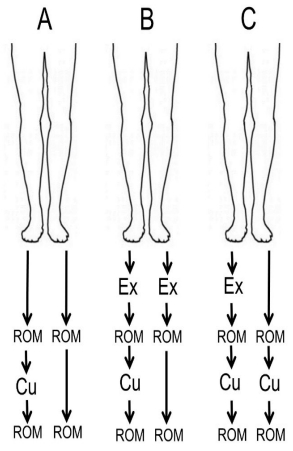
Participants self-reported age, height, and weight after which they were counterbalanced by gender and randomly placed in one of three groups: A, B, or C. Group A did not perform any heel drops but received one bout of the cupping protocol on the right gastrocnemius region (calf), group B performed heel drops on the right and left side but received cupping on the right side only, and group C performed heel drops on the right side only and received cupping on both claves <Figure 1>.
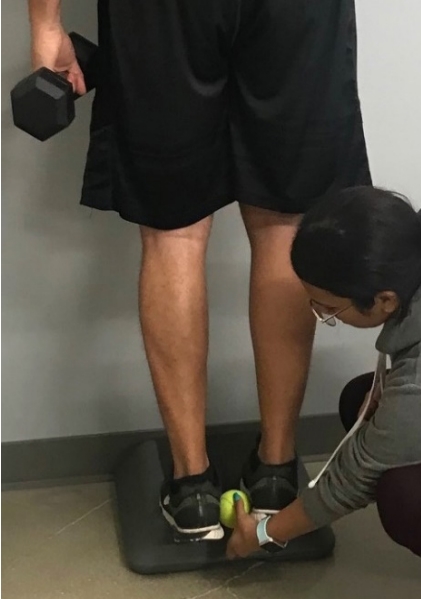
Group B performed heel drops with both ankles using a tennis ball between the medial heels of the shoes to ensure uniformity of movement <Figure 2>. Group C performed heel drops only on the right side while group A did not perform heel drops at all.
The heel drop protocol used to elicit DOMS is similar to that used in a previous study [39]. Participants performed heel drops on a standard riser while facing a wall with a mounted bar approximately chest-height. With the right hand grasping the bar, participants assisted themselves up during plantar flexion before eccentrically dorsiflexing. Participants were required to eccentrically dorsiflex below the ankle as far as possible. A 2.26 kg (5-lb, females) or 4.53 kg (10-lb males) weight was held in the left hand while completing the heel drops at a cadence of 70 beats per minute using a metronome, where a beat signaled participants to plantarflex and the next beat signaled participants to dorsiflex. This was continued until participants could no longer continue or until they were no longer moving through a full range of motion, which was characterized by the heel not lowering below the ankle. At this point a one-minute rest was provided after which participants repeated the exercise again in the same manner, but without the weight. A 5-minute rest was then given prior to cupping.
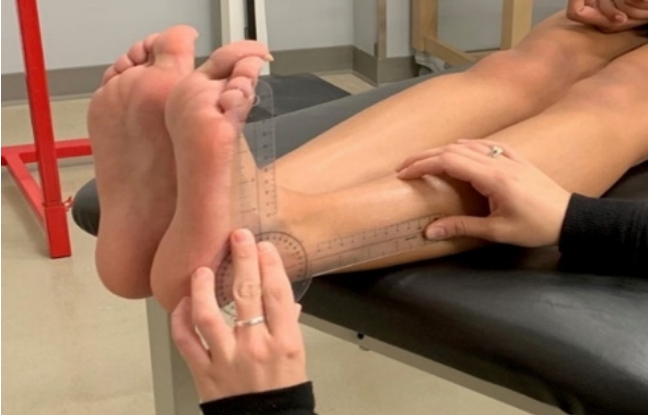
Range of motion (ROM) of the ankle was measured in all groups during the 5-min rest prior to cupping and immediately again after cupping in both ankles regardless of performing the heel drops. Participants sat on an exam table with knees extended and the ankle hanging over the edge with shoes and socks removed. Active dorsiflexion of each ankle was measuring with a goniometer <Figure 3> using the fibular head and fifth metatarsal as the proximal and distal landmarks respectively. The respective sides of the goniometer were aligned with the appropriate landmarks while the participant actively dorsiflexed the ankle.
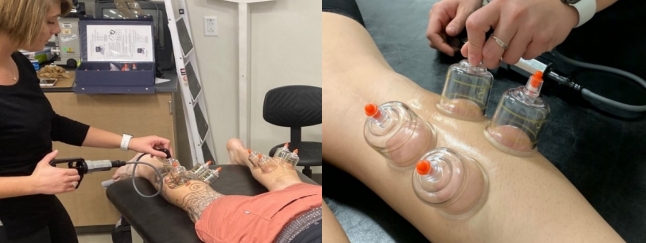
When the five-minute rest was complete, one bout of the cupping protocol was conducted on the right gastrocnemius region <Figure 4> (A. G. Professional Cupping Set; K.S. Choi Corp, California, USA). Preparation of the quadrants included removal of all hair, light abrasion with 70% isopropyl alcohol swabs, and lastly applying olive oil for aid in the seal of the cups to ensure suction. Two-inch diameter cups were placed in each quadrant (right and left, upper and lower) with the intensity of one full pump. Once all four cups were providing suction, a timer was started for 90 seconds, after which the cups were gently removed and excess olive oil was then wiped away using a paper towel.
Participants then turned over on the exam table at which time ROM was again measured in the same manner as described above. They were reminded to avoid any anti-inflammatory or pain reducing medications and supplements, and to carry on their normal daily physical activities but to avoid exercise of any kind involving the lower extremities. A visual analog soreness scale (VAS) of 0 (no soreness at all) to 10 (unable to move) was explained and provided to participants, after which they reported at 24- and 48-hrs after cupping. Scales such as this have been assessed for good reliability [40].
SPSS v25 was used to run all statistical analyses. A 3 (group) x 4 (soreness) Factorial ANOVA with repeated measures on the second factor was used to assess calf soreness at 24- and 48-hours between the three groups for DOMS as well as for ROM. FisherŌĆÖs Least Squared Difference was used to control type I error in post-hoc tests. Effect sizes of post-hoc tests were calculated with CohenŌĆÖs d using the pooled standard deviation, with 0.8 or greater considered a large effect, 0.5 a moderate effect, and 0.2 or less a small effect. Alpha was set at 0.05 for all tests.
Eighteen male and 18 female participants enrolled and completed the study. Participant characteristics are reported in Table 1.
Factorial ANOVA indicated a significant interaction between groups and time (F(6, 64), = 5.4, p = 0.001, ╬Ęp2 = .34).
At 24 hours, there was a significant difference in left calf soreness between groups A and B (p = 0.001, d = 3.8) and between B and C (p = 0.001, d = 3.2). This was also evident at the same time-point for right calf soreness between group A and group B (p = 0.001, d = 3.1) as well as groups A and C (p = 0.001, d = 2.2) <Table 2>.
There was a significant difference in left calf soreness at 48 hours between group A and group B (p = 0.001, d = 2.9) and between groups B and C (p = 0.001, d = 2.8). Right calf soreness at 48 hours was also significantly different between group A and group B (p = 0.001, d = 2.2) as well as groups A and C (p = 0.001, d = 1.4) <Table 2>. No significant difference existed between the left calf of group B and the right calf of group C at 24 (p = 0.166, d = 0.6) and 48 hours (p = 0.408, d = 0.3).
No significant differences were found in soreness between right and left calves in group A at 24 hours (p = 0.616, d =0.4) and 48 hours (p = 0.476, d = 0.0). A significant difference existed between calves for group B at 24 hours (p = 0.029, d = 0.6), but not 48 hours (p = 0.388, d = 0.2). Finally, a significant difference between right and left calves was found at both 24 hours (p = 0.001, d = 2.1) and 48 hours (p = 0.001, d =1.4) for group C <Table 2>.
There was no interaction of group and calf on ROM (F(6, 64), = 0.685, p = 0.662, ╬Ęp2 = 0.06) <Figure 5>, nor was there a main effect of group when time was combined (F(2, 33), = 0.182 p = 0.835, ╬Ęp2 = 0.01). There was, however, a significant difference for the main effect of time when group was combined (F(3, 33), = 7.78, p = 0.001, ╬Ęp2 = 0.41) Post-hocs indicated a significant difference between left and right calves at 24 hours (p = 0.001, d = 0.26) and between 24 and 48 hours in the left calf (p = 0.007, d = 0.19).
This study investigated the effect of dry cupping therapy on muscle soreness and ROM after a bout of eccentric dorsiflexion exercise. The only significant finding was in soreness rating between the left and right calves at 24 hrs in group B (3.58┬▒1.31 and 2.83┬▒1.03 VAS units, respectively), in which both calves were exercised and only the right side was cupped. While this provides some evidence for 90 seconds of dry cupping to acutely reduce the perception of muscle soreness, uncertainty still exists since there was a significant difference in soreness between right and left calves in group C, both of which were cupped but only the right exercised. Furthermore, there was no significant difference in soreness at either time point between the right calves of group B and the left calves of group C, both of which were exercised but only cupped on group C. All other significant findings simply demonstrate the effectiveness of the heel drop protocol to induce soreness.
There is evidence to show that dry cupping can increase microvascular function [41] thereby promoting blood and lymphatic flow with negative pressure from suction, which causes stretching of the skin and underlying tissue as well as dilation of the capillaries [42]. It can be theorized this local effect of increased flow could lead to shorter healing times with decreased pain, however, studies that support claims of dry cupping for improving pain relief are equivocal. For example, after 71 participants with heel pain were divided into a treatment and control group, they performed active dorsiflexion and self-stretching exercises with the treatment group receiving dry cupping on trigger points during these exercises. Total cupping time for the treatment group was 10 minutes. Immediately after the intervention, pain as measured with a VAS was significantly lower compared to pre-measurement, but not between groups, nor were there any significant differences 48-hrs later [29]. The authors also measured heel pain during the first morning steps one and two days after the intervention, and reported that pain in the treatment group was significantly less than that in the control group. Other studies have provided evidence of pain improvement after dry cupping in other areas of the body. After 60 participants with existing neck and shoulder pain received 10 minutes of dry cupping, pain as measured with a VAS was significantly reduced compared to a control group immediately after the treatment [43]. Five minutes of dry cupping seems to significantly increase pain threshold in healthy hamstring muscles from pre- to post-treatment, although this increase was not significant compared to a control group that engaged in passive stretching [31]. For those with low back pain, eight minutes of cupping twice weekly for four weeks with either higher or lower suction pressure significantly improved their perception of pain [44]. As with the above mentioned studies, this study found mixed results with some evidence of cupping to reduce soreness over a shorter, but not longer term, albeit only within-subjects and not across groups. It has been suggested that one means by which dry cupping can reduce pain is similar to acupressure and acupuncture, in that dry cupping can elicit the release of endorphins and other pain relief substances [45]. Perhaps 90 seconds of cupping is not long enough to elicit physiological responses that includes sufficient capillary dilation and endorphin stimulation for longer-term pain relief. Reasons for mixed results in this and other studies are most likely due to a non-definitive methodology for cupping, as cupping has been explored using different time exposures, different types of dry cupping (different negative pressures, pulsatile, flame suction, different size cups), different parts of the body, and different populations.
The current study indicates that 90-seconds of dry cupping after a bout of eccentric heel drop exercise does not enhance ROM of the ankle joint. Although the main effect of time was significant, this may be attributed to the exercise protocol and possible tightness of the calf muscles since there is very little indication that cupping had any effect. A limitation of this study, however, is that ROM was not assessed before the exercise condition and therefore the effect of the heel drop exercise on ROM cannot be determined. It is possible that the heel drop exercise did not have an influence of ROM in either group B or C, thereby not effecting a significant change between the two post-exercise ROM assessments. If ROM never changed from baseline, then dry cupping could not have had an influence.
There is evidence, however, that dry cupping can influence ROM. For example, it has been reported that dry cupping while performing ankle dorsiflexion exercises and calf muscle stretching significantly improved ankle dorsiflexion ROM immediately after and two days after the intervention in both treatment and control groups [29]. While the control group performed the same exercises and stretches as the treatment group, but without the cupping, there was no significant difference between the groups. This is similar to studies examining other areas of the body, such as when 15 healthy adults received dry cupping on the hamstrings for five minutes and a control group engaged in passive stretching. Statistically significant improvements from pre- to post-testing in both treatment and passive stretching groups were evident, but no significant difference existed between the groups [31]. This suggests that cupping can increase ROM but is not superior to traditional passive stretching. Similarly, 17 collegiate athletes with a hamstring pathology were given three minutes of cupping and like the aforementioned study, there was a significant improvement in ROM from pre-to post-testing but no significant difference between the group that received cupping and the group that received heat treatment and foam rolling [46]. In contrast, when 25 healthy young adults engaged in dry cupping, sham, and control trials and assessed hamstring ROM, there were no significant differences in ROM measures immediately post and 10-mins post cupping between the trials, which suggested that dry cupping did not impact flexibility [47]. In another study, 25 young adult collegiate athletes were given either a 7-minute cupping therapy on the hamstrings or assigned to a control group with no treatment at all. Similar to the last study, there were no significant differences in ROM for pre- and post-testing between groups, thus indicating dry cupping did not affect hamstring ROM [48]. The current study is the first known investigation of exploring cuppingŌĆÖs effects on ROM after an eccentric bout of exercise in the calf region. Similar to the above mentioned studies, there was no improvement in ROM for within (pre- to post-test) or between (cupped and non-cupped) trails. While differences in methodology must be accounted for, such as duration of cupping, sites being cupped, techniques used to measure outcome variables, etc., it is likely that 90 seconds of dry cupping as a primary means to increase ROM may not be effective after a bout of eccentric heel drop exercise.
Limitations of this study include the novel cupping protocol. The aim of this study was to determine if an acute (90 seconds) bout of cupping could provide relief from soreness and since no other studies have used such a short bout, no direct comparisons can be made. Since this protocol has not been assessed against repeated trials or a gold standard for muscle soreness relief, there is no information for its reliability or validity. The lack of sham cupping is also a limitation. Without a sham treatment, it was obvious to participants which calves were and were not cupped and therefore could have influenced the way they rated soreness. The 10-pt VAS can be considered another limitation in that it was developed for rating pain and not muscle soreness. Soreness, similar to pain, can be subjective and some may perceive it as a discomfort. Additionally, this study is limited such that there is no direct physiological evidence that DOMS occurred since markers of muscle damage were not collected.
Whether one is an athlete or a patient undergoing physical therapy, muscle soreness can be a hindrance in training and rehabilitation programs, and ways to reduce this condition are continually explored. Results from this study indicate that while 90 seconds of dry cupping on the calf may reduce 24-hr muscle soreness after performing heel drops to exhaustion, there is little evidence otherwise to suggest its effectiveness for lowering muscle soreness in the calf or increasing ROM in the ankle. This is the first study known to the authors to explore the effect of dry cupping on muscle soreness in the calf. Future studies can incorporate a longer suction periods, such as three to 10 minutes as commonly found in other studies. Further research can also include sham cupping, which may be effective in hiding the treatment, especially in those who have never experienced cupping.
Figure┬Ā1.
Participants in group B performed heel drop exercise (Ex) on both sides while participants in group C performed heel drop exercises on the right side, and participants in groups A and B received cupping (Cu) on the right side only while those in group C received it on both sides. Range of motion (ROM) was measured in all ankles prior to and after the cupping.
Figure┬Ā3.
A standard goniometer was used to measure dorsiflexion of the ankle joint using the fibular head and fifth metatarsals as bony landmarks to ensure accuracy.
Figure┬Ā4.
One bout of the cupping protocol being administered to a participant. One suction to the four quadrants was held for 90 seconds.
Figure┬Ā5.
There were no significant differences in ankle range of motion between calves within groups nor between calves across groups before and after cupping, p > .05.

Table┬Ā1.
Participant characteristics (mean┬▒standard deviation)
Table┬Ā2.
Soreness ratings using a 10-point visual analog scale after calf exercise and cupping (mean┬▒standard deviation).
| Group A (No exercise, right calf cupped) | Group B (Bilateral exercise, right calve cupped) | Group C (Right calf exercise, bilateral cupped) | |
|---|---|---|---|
| 24-hr Left Calf | 0.00┬▒0.00 | 3.58┬▒1.31ad | 0.25┬▒0.62b |
| 24-hr Right Calf | 0.16┬▒0.57 | 2.83┬▒1.02a | 2.66┬▒1.49a |
| 48-hr Left Calf | 0.00┬▒0.00 | 3.50┬▒1.67c | 0.08┬▒0.28b |
| 48-hr Right Calf | 0.00┬▒0.00 | 3.08┬▒1.92c | 2.66┬▒2.53c |
References
1. Gulick DT, Kimura I F. Delayed onset muscle soreness: What is it and how do we treat it? J Sport Rehab. 1996; 5(3): 234ŌĆō243.

2. Armstrong RB. Mechanisms of exercise-induced delayed onset muscular soreness: a brief review. Med Sci Sports and Exerc. 1984; 16(6): 529ŌĆō538.
3. Cheung K, Hume PA, Maxwell L. Delayed onset muscle soreness. Treatment strategies and performance factors. Sports Med. 2003; 33(2): 145ŌĆō164.

4. Clarkson PM, Nosaka K, Braun B. Muscle function after exercise-induced muscle damage and rapid adaptation. Med Sci Sport Exerc. 1992; 24(5): 512ŌĆō520.

5. Cleak MJ, Eston RG. Muscle soreness, swelling, stiffness and strength loss after intense eccentric exercise. Br J Sports Med. 1992; 26(4): 267ŌĆō272.



6. Connolly DA, Sayers SP, McHugh MP. Treatment and prevention of delayed onset muscle soreness. J Strength and Cond Res. 2003; 17(1): 197ŌĆō208.

7. Dutto DJ, Braun WA. DOMS-Associated changes in ankle and knee joint dynamics during running. Med Sci Sport Exerc. 2004; 36(4): 560ŌĆō566.

8. Newham D. The consequences of eccentric contractions and their relationship to delayed onset muscle pain. Eur J Appl Physiol Occup Physiol. 1988; 57(3): 353ŌĆō359.


9. Paschalis V, Giakas G, Baltzopoulos V, et al. The effects of muscle damage following eccentric exercise on gait biomechanics. Gait Posture. 2007; 25(2): 236ŌĆō242.


10. Larkin-Kaiser KA, Parr JJ, Borsa PA, George SZ. Range of motion as a predictor of clinical shoulder pain during recovery from delayed-onset muscle soreness. J Athl Train. 2015; 50(3): 289ŌĆō294.



11. Weber MD, Servedio FJ, Woodall WR. The effects of three modalities on delayed onset muscle soreness. J Orthop Sports Phys Ther. 1994; 20(5): 236ŌĆō242.


13. Lewis BB, Ruby D, Bush-Joseph C A. Muscle soreness and delayed-onset muscle soreness. Clin Sports Med. 2021; 31(2): 255ŌĆō262.

14. Tokinoya K, Ishikura K, Song-Gyu R, Ebina K, Miyakawa S, Ohmori H. Relationship between early-onset muscle soreness and indirect muscle damage markers and their dynamics after a full marathon. J Exercise Sci Fit. 2020; 18(3): 115ŌĆō121.

15. Khataei T, Harding AMS, Janahmadi M, et al. ASICs are required for immediate exercise-induced muscle pain and are downregulated in sensory neurons by exercise training. J Appl Physiol. 2020; 129(1): 17ŌĆō26.


16. Khataei T, Sluka K, Harding A, Benson C. ASICs are required for immediate exercise-induced muscle pain (IEIP), but not delayed onset muscle soreness (DOMS). J of Pain. 2021; 22(5): 591.

17. Hilbert JE, Sforzo GA, Swensen T. The effects of massage on delayed onset muscle soreness. Br J Sports Med. 2003; 37(1): 72ŌĆō75.



18. Rodenburg JB, Steenbeek D, Schiereck P, B├żr PR. Warmup, stretching and massage diminish harmful effects of eccentric exercise. Int J Sports Med. 1994; 15(7): 414ŌĆō419.


19. Behm DG, Blazevich AJ, Kay AD, McHugh M. Acute effects of muscle stretching on physical performance range of motion, and injury incidence in healthy active individuals: a systematic review. Appl Physiol Nutr Metab. 2016; 41(1): 1ŌĆō11.


20. Kelly S, Beardsley C. Specific and cross-over effect of foam rolling on ankle dorsiflexion range of motion. Int J Sports Phys Ther. 2016; 11(4): 544ŌĆō551.


21. Laffaye G, Da Silva DT, Delafontaine A. Self-myofascial release effect with foam rolling on recovery after high-intensity interval training. Front Physiol. 2019; 10:1287.



22. Ahmedov S. Ergogenic effect of acupuncture in sport and exercise: a brief review. J Strength and Cond Res. 2010; 24(5): 1421ŌĆō1427.

23. Hubscher M, Vogt L, Bernhorsten M, Rosenhagen A, Banzer W. Effects of acupuncture on symptoms and muscle function in delayed-onset muscle soreness. J Altern Complement Med. 2008; 14(8): 1011ŌĆō1016.


24. Itoh K, Ochi H, Kitakohi H. Effect of tender point acupuncture on delayed onset muscle soreness (DOMS)-a pragmatic trial. Chin Med. 2008; 3(14): 1ŌĆō5.


25. Hill JM, Sumida KD. The effect of 2 topical counterirritant creams on pain induced by delayed-onset muscle soreness. J Sport Rehabil. 2002; 11(3): 202ŌĆō208.

26. Jamurtas AZ, Fatouros IG, Buckenmeyer P, et al. Effects of plyometric exercise on muscle soreness and plasma creatine kinase levels and its comparison with eccentric and concentric exercise. J Strength and Cond Res. 2000; 14(1): 68ŌĆō74.

27. Cao H, Han M, Li X, et al. Clinical research evidence of cupping therapy in China: a systematic literature review. BMC Complement Altern Med. 2010; 10(70).

28. Akbarzadeh M, Ghaemmaghami M, Yazdanpanahi Z, Zare N, Azizi A. The effect dry cupping therapy at acupoint BL23 on the intensity of postpartum low back pain in primiparous women based on two types of questionnaires, 2012; a randomized clinical trial. Int J Community Based Nurs Midwifery. 2014; 2(2): 112ŌĆō120.


29. AlKhadhrawi NA, Alshami A. Effects of myofascial trigger point dry cupping on pain and function in patients with plantar heel pain: a radomized controlled trial. J Bodyw Mov Ther. 2019; 23(3).
30. Arce-Esquivel AA, Warner BJ, Gallegos DM, Cage SA. Effect of dry cupping on vascular function among young individuals. Int J Health Sci. 2017; 5(3): 10ŌĆō15.
31. Kim J, Cho JE, Do KS, Lim SY, Kim HJ, Yim J. Effect of cupping therapy on range of motion, pain threshold, and muscle activity of the hamstring muscle compared to passive stretching. J Korean Soc Phys Med. 2017; 12(3): 23ŌĆō32.

32. Kim JI, Lee MS, Lee DH, Boddy K, Ernst E. Cupping for treating pain: systematic review. Evid Based Complement Alternat Med. 2011; 2011(467014).
33. Lauche R, Cramer H, Choi KE, et al. The influence of a series of five dry cupping treatments on pain and mechanical thresholds in patients with chronic nonspecific neck pain-a randomised controlled pilot study. BMC Complement Altern Med. 2011; 11(63).

34. Lauche R, Cramer H, Hohmann C, et al. The effect of traditional cupping on pain and mechanical thresholds in patients with chronic nonspecific neck pain: a randomised controlled pilot study. Evid Based Complement Alternat Med. 2012; 2012(429718).

35. Murray D, Clarkson C. Effects of moving cupping therapy on hip and knee range of movement and knee flexion power: a preliminary investigation. J Man Manip Ther. 2019; 27(5): 287ŌĆō294.



36. Bridgett R, Klose P, Duffield R, Mydock S, Lauche R. Effects of cupping therapy in amateur and professional athletes: systematic review of randomized controlled trials. J Altern Complement Med. 2018; 24(3): 208ŌĆō219.


37. Charles D, Hudgins T, MacNaughton J, Newman E, Tan J. A systematic review of manual therapy techniques, dry cupping and dry needling in the reduction of myofascial pain and myofascial trigger points. J Bodyw Mov Ther. 2019; 23(3): 539ŌĆō546.


38. Faul F, Erdfelder E, Lang AG, Buchner A. G*Power 3: A flexible statistical power analysis program for the social, behavioral, and biomedical sciences. Behav Res Methods. 2007; 39(2): 175ŌĆō191.


39. Heiss R, Hotfiel T, Kellermann M, et al. Effect of compression garments on the development of edema and soreness in delayed-onset muscle soreness (DOMS). J Sports Sci Med. 2018; 17(3): 392ŌĆō401.


40. Bijur PE, Silver W, Gallagher EJ. Reliability of the visual analog scale for measurement of acute pain. Acad Emerg Med. 2001; 8(12): 1153ŌĆō1157.


41. Al-Bedah AMN, Elsubai IS, Qureshi NA, et al. The medical perspective of cupping therapy: effects and mechanisms of action. J Tradit Complement Med. 2019; 9(2): 90ŌĆō97.


42. Lowe DT. Cupping therapy: An analysis of the effects of suction on skin and the possible influence on human health. Complement Ther Clin Pract. 2017; 29:162ŌĆō168.


43. Chi LM, Lin LM, Wang SF, Lai HL, Peng TC. The effectiveness of cupping therapy on relieving chronic neck and shoulder pain: A randomized controlled trial. Evid Based Complement Alternat Med. 2016; 2016(73589180).

44. Teut M, Ullman A, Ortiz M, et al. Pulsatile dry cupping in chronic low back pain - A randomized three-armed controlled clinical trial. BMC Complement Altern Med. 2018; 18(1): 115.



45. Rozenfeld E, Kalichman L. New is the well-forgotten old: The use of dry cupping in musculoskeletal medicine. J Bodyw Mov Ther. 2016; 20(1): 173ŌĆō178.


46. Warren AJLZ, Volberding JM, OŌĆÖBrien MS. Treatment outcomes of myofascial decompression (cupping therapy) on hamstring pathology. J Athl Train. 2017; 52(6 Supplement):SŌĆō97.